Abstract
Background
Surgical mesh is widely used not only to treat but also to prevent incisional hernia formation. Despite much effort by material engineers, the 'ideal' mesh mechanically, biologically and surgically easy to use remains elusive. Advances in tissue engineering and nanomedicine have allowed new concepts to be tested with promising results in both small and large animals. Abandoning the concept of a pre-formed mesh completely for a ‘pour in liquid mesh’ has never been tested before.
Materials and methods
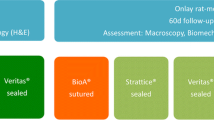
Thirty rabbits underwent midline laparotomy with closure using an absorbable suture and small stitch small bites technique. In addition, their abdominal wall closure was reinforced by a liquid nanofibrous scaffold composed of a fibrin sealant and nanofibres of poly-ε-caprolactone with or without hyaluronic acid or the sealant alone, poured in as an ‘onlay’ over the closed abdominal wall. The animals were killed at 6 weeks and their abdominal wall was subjected to histological and biomechanical evaluations.
Results
All the animals survived the study period with no major complication. Histological evaluation showed an eosinophilic infiltration in all groups and foreign body reaction more pronounced in the groups with nanofibres. Biomechanical testing demonstrated that groups treated with nanofibres developed a scar with higher tensile yield strength.
Conclusion
The use of nanofibres in a liquid form applied to the closed abdominal wall is easy to use and improves the biomechanical properties of healing fascia at 6 weeks after midline laparotomy in a rabbit model.




Similar content being viewed by others
References
Fink C, Baumann P, Wente MN et al (2014) Incisional hernia rate 3 years after midline laparotomy. Br J Surg 101:51–54
Henriksen NA, Montgomery A, Kaufmann R, Berrevoet F, East B, Fischer J, Hope W, Klassen D, Lorenz R, Renard Y, Garcia Urena MA, Simons MP, European and Americas Hernia Societies (EHS and AHS) (2020) Guidelines for treatment of umbilical and epigastric hernias from the European Hernia Society and Americas Hernia Society. BJS 107(3):171–190
The Hernia Surge Group (2018) International guidelines for groin hernia management. Hernia 22:1–165
San Miguel C, Melero D, Jiménez E, López P, Robin A, Blázquez LA, López-Monclús ML, González E, Jiménez C, García-Ureña MA (2018) Long-term outcomes after prophylactic use of onlay mesh in midline laparotomy. Hernia 22(6):1113–1122
Jairam AP, Timmermans L, Eker HH, Pierik RM, van Klaveren D, Steyerberg EW, Timman R, van der Ham AC, Dawson I, Charbon JA, Schuhmacher C, Mihaljevic A, Izbicki JR, Fikatas P, Knebel P, Fortelny RH, Kleinrensink GJ, Lange JF, Jeekel HJ (2017) Prevention of incisional hernia with prophylactic onlay and sublay mesh reinforcement versus primary suture only in midline laparotomies (PRIMA): 2-year follow-up of a multicentre, double-blind, randomised controlled trial. Lancet 390(10094):567–576
Plencner M, East B, Tonar Z, Otáhal M, Prosecká E, Rampichová M, Krejčí T, Litvinec A, Buzgo M, Míčková A, Nečas A, Hoch J, Amler E (2014) Abdominal closure reinforcement by using polypropylene mesh functionalized with poly-ε-caprolactone nanofibers and growth factors for prevention of incisional hernia formation. Int J Nanomed 9(9):3263–3277
Vozzi F, Nardo T, Guerrazzi I, Domenici C, Rocchiccioli S, Cecchettini A, Comelli L, Vozzi G, De Maria C, Montemurro F, Ciardelli G, Chiono V (2018) Integration of biomechanical and biological characterization in the development of porous poly(caprolactone)-based membranes for abdominal wall hernia treatment. Int J Pol Sci 2018:1–15
Cipitria A, Skelton A, Dargaville TR, Daltonac PD, Hutmacher DW (2011) Design, fabrication and characterization of PCL electrospun scaffolds—a review. J Mater Chem 21:9419–9453
East B, Plencner M, Kralovic M, Rampichova M, Sovkova V, Vocetkova K, Otahal M, Tonar Z, Kolinko Y, Amler E, Hoch J (2018) A polypropylene mesh modified with poly-ε-caprolactone nanofibers in hernia repair: large animal experiment. Int J Nanomed 28(13):3129–3143
Collins MN, Birkinshaw C (2013) Hyaluronic acid based scaffolds for tissue engineering—a review. Carbohyd Polym 92(2):1262–1279
Plencner M, Prosecká E, Rampichová M, East B, Buzgo M, Vysloužilová L, Hoch J, Amler E (2015) Significant improvement of biocompatibility of polypropylene mesh for incisional hernia repair by using poly-ε-caprolactone nanofibers functionalized with thrombocyte-rich solution. Int J Nanomed 10:2635–2646
Jakubova R, Mickova A, Buzgo M, Rampichova M, Prosecka E, Tvrdik D, Amler E (2011) Immobilization of thrombocytes on PCL nanofibres enhances chondrocyte proliferation in vitro. Cell Prolif 44(2):183–191
Vocetkova K, Buzgo M, Sovkova V, Bezdekova D, Kneppo P, Amler E (2016) Nanofibrous polycaprolactone scaffolds with adhered platelets stimulate proliferation of skin cells. Cell Prolif 49(5):568–578
Cao H, McHugh K, Chew SY, Anderson JM (2010) The topographical effect of electrospun nanofibrous scaffolds on the in vivo and in vitro foreign body reaction. J Biomed Mater Res A 93(3):1151–1159
Burger JW, Lange JF, Halm JA, Kleinrensink GJ, Jeekel H (2005) Incisional hernia: early complication of abdominal surgery. World J Surg 29(12):1608–1613
Harlaar JJ, Deerenberg EB, Dwarkasing RS, Kamperman AM, Kleinrensink GJ, Jeekel J, Lange JF (2017) Development of incisional herniation after midline laparotomy. BJS Open 1(1):18–23
Li S, Liu L, Garreau H, Vert M (2003) Lipase-catalyzed biodegradation of poly(ε-caprolactone) blended with various polylactide-based polymers. Biomacromol 4(2):372–377
Azimi B, Nourpanah P et al (2014) Poly (ε-caprolactone) fiber: an overview. J Eng Fibers Fabr 9(3):74–90
Coden ME, Loffredo LF, Walker MT, Jeong BM, Nam K, Bochner BS, Abdala-Valencia H, Berdnikovs S (2020) Fibrinogen is a specific trigger for cytolytic eosinophil degranulation. J Immunol 204(2):438–448
Kramer M, Font E (2017) Reducing sample size in experiments with animals: historical controls and related strategies. Biol Rev 92:431–445
Sarver DC, Kharaz YA, Sugg KB, Gumucio JP, Comerford E, Mendias CL (2017) Sex differences in tendon structure and function. J Orthopaedic Res 35:2117–2126
Acknowledgements
The author team would like to thank Doc MVDr Josef Illek DrSc Dipl ECBHM from University of Veterinary and Pharmaceutical Sciences in Brno, Czech Republic and doc RNDr Ján Sabo, CSc from University Centre for Energy Efficient Buildings, Czech Technical University in Prague for their support and mentorship thought the course of the experiment.
Funding
This research has been supported by a grant from the Czech Health Research Council Reg No. 17-32285A and by a research grant from the European Hernia Society.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We were uploaded for each author individually.
Ethical approval
All procedures performed within this study were approved by the Ministry of Education of the Czech republic (approval no.11921/2017-4) and were in accordance with the Euroepan Union ethical standards for animal reserach.
Human and animal rights
We have confirmed to the Act. No. 246/1992 Coll., as amended, and Decree No. 419/2012 Coll., on the protection of experimental animals.
Informed consent
We do not have informed consent as this is an animal trial.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Abstract submitted to Hernia21, the Annual Congress of the European Hernia Society, Copenhagen, October 2021 and has won the BJS hernia prize.
Supplementary Information
Below is the link to the electronic supplementary material.
10029_2022_2582_MOESM1_ESM.docx
Supplementary file1 (DOCX 86 KB) Supplementary Fig. 1 1a: Particle size distribution of milled PCL/HA+PL scaffold. 1b Distribution of fibre diameter size of PCL nanofibre scaffold. 1c Distribution of fibre diameter size of PCL/HA nanofibre scaffold. Particle size distribution after milling process was distributed according to log-normal distribution with peak in a range of 10 µm to 20 µm. The size of individual particles was determined as twice the semi-major axis of ellipse fitted to the measured particle. The measured particles in the range of 10 µm to 20 µm made up only 3 % to 5 % of total particles mass in the prepared sample. The milling process, particle surface morphology, nanofibre surface chemistry, humidity and chemistry of the environment caused many of the small milled particles to connect to create cluster like larger particles with nanofibre structure
10029_2022_2582_MOESM3_ESM.docx
Supplementary file3 (DOCX 188 KB) Supplementary Figure 3 Tissue composition of surgical wound. Boxplot of percentage of connective tissues (dense and loose together). (I - Artiss, II - PCL+Artiss, III - PCL/hPL+Artiss, IV - PCL/HA+Artiss, V - PCL/HA+hPL+Artiss)
10029_2022_2582_MOESM4_ESM.docx
Supplementary file4 (DOCX 13 KB) Supplementary Table 2 Standard T-test to determine statistical signifikance of the difference between the elastic modulus and dissipative energy density of group IV compared to other groups.
Rights and permissions
About this article
Cite this article
East, B., Woleský, J., Divín, R. et al. Liquid resorbable nanofibrous surgical mesh: a proof of a concept. Hernia 26, 557–565 (2022). https://doi.org/10.1007/s10029-022-02582-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-022-02582-1