Abstract
Background
An indication for selective shunting during carotid endarterectomy (CEA) is based on monitoring during a procedure. Cerebral oximetry (CO) using near-infrared spectroscopy (NIRS) may be a simple technique, but its relevance during CEA, especially with respect to cutoff values indicating shunt implantation, still needs to be elucidated.
Methods
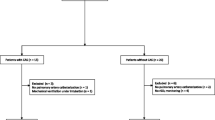
One hundred twenty five patients underwent CEA under local anesthesia (LA) and were monitored clinically throughout the whole procedure. The patients were also monitored using bilateral NIRS probes during surgery. The NIRS values were recorded and evaluated before and after selective cross-clamping, firstly by the external carotid artery (ECA), followed by the internal carotid artery (ICA). The decrease in the ipsilateral CO values, with respect to the indication of shunting, was only analyzed after selective cross-clamping of the ICA. The decision to use an intraluminal shunt was solely based on the neurological status evaluation after ICA cross-clamping.
Results
One hundred five patients (85%) were stable throughout the CEA, while 20 patients (15%) clinically deteriorated during surgery. The mean drop in the CO after selective ICA clamping in clinically stable patients was 6%, while in patients with clinical deterioration, the NIRS decreased by 14.5% (p < 0.05). When the cutoff value for selective shunting was set as a 10% decrease of the ipsilateral CO after selective ICA clamping, the sensitivity of the technique was 100% and the specificity 83.0%.
Conclusions
Our study showed that a 10% decrease in the ipsilateral brain tissue oximetry after selective cross-clamping the ICA provides a reliable cutoff value for selective shunting during CEA. Despite the availability of a variety of monitoring tools, the NIRS may be an easy, reliable option, especially in the scenario of acute CEA in general anesthesia.




Similar content being viewed by others
References
AbuRahma AF, Metz MJ, Robinson PA (2003) Natural history of > or =60% asymptomatic carotid stenosis in patients with contralateral carotid occlusion. Ann Surg 238:551–561 discussion 561-552
Ali AM, Green D, Zayed H, Halawa M, El-Sakka K, Rashid HI (2011) Cerebral monitoring in patients undergoing carotid endarterectomy using a triple assessment technique. Interact Cardiovasc Thorac Surg 12:454–457
American College of Cardiology Foundation/American Heart Association Task F, American Stroke A, American Association of Neuroscience N, American Association of Neurological S, American College of R, American Society of N, Congress of Neurological S, Society of Atherosclerosis I, Prevention, Society for Cardiovascular A, Interventions et al (2011) 2011 asa/accf/aha/aann/aans/acr/asnr/cns/saip/scai/sir/snis/svm/svs guideline on the management of patients with extracranial carotid and vertebral artery disease: executive summary. J Neurointerv Surg 3:100–130
Bond R, Rerkasem K, Counsell C, Salinas R, Naylor R, Warlow CP, Rothwell PM (2002) Routine or selective carotid artery shunting for carotid endarterectomy (and different methods of monitoring in selective shunting). Cochrane Database Syst Rev CD000190
Calligaro KD, Dougherty MJ (2005) Correlation of carotid artery stump pressure and neurologic changes during 474 carotid endarterectomies performed in awake patients. J Vasc Surg 42:684–689
CASMED Field service manual. Fore-sight_mc-2000 series cerebral oximeter. https://www.manualslib.com/manual/1221626/Casmed-Fore-Sight-Elite.html (accessed Apr 28, 2020)
Congruksut W, Vaniyapong T, Rerkasem K (2014) Routine or selective carotid artery shunting for carotid endarterectomy (and different methods of monitoring in selective shunting). Cochrane Database Syst Rev CD000190
Davie SN, Grocott HP (2012) Impact of extracranial contamination on regional cerebral oxygen saturation: a comparison of three cerebral oximetry technologies. Anesthesiology 116:834–840
Domenick Sridharan N, Thirumala P, Chaer R, Balzer J, Long B, Crammond D, Makaroun M, Avgerinos E (2018) Predictors of cross-clamp-induced intraoperative monitoring changes during carotid endarterectomy using both electroencephalography and somatosensory evoked potentials. J Vasc Surg 67:191–198
Giles MF, Rothwell PM (2005) The need for emergency treatment of transient ischemic attack and minor stroke. Expert Rev Neurother 5:203–210
Group GTC, Lewis SC, Warlow CP, Bodenham AR, Colam B, Rothwell PM, Torgerson D, Dellagrammaticas D, Horrocks M, Liapis C, Banning AP et al (2008) General anaesthesia versus local anaesthesia for carotid surgery (gala): a multicentre, randomised controlled trial. Lancet 372:2132–2142
Guay J, Kopp S (2013) Cerebral monitors versus regional anesthesia to detect cerebral ischemia in patients undergoing carotid endarterectomy: a meta-analysis. Can J Anaesth 60:266–279
Hans SS, Jareunpoon O (2007) Prospective evaluation of electroencephalography, carotid artery stump pressure, and neurologic changes during 314 consecutive carotid endarterectomies performed in awake patients. J Vasc Surg 45:511–515
Hyttel-Sorensen S, Hessel TW, Greisen G (2014) Peripheral tissue oximetry: comparing three commercial near-infrared spectroscopy oximeters on the forearm. J Clin Monit Comput 28:149–155
Jonsson M, Lindstrom D, Wanhainen A, Djavani Gidlund K, Gillgren P (2017) Near infrared spectroscopy as a predictor for shunt requirement during carotid endarterectomy. Eur J Vasc Endovasc Surg 53:783–791
Kakkos SK, Tsolakis IA (2017) Commentary on “near infrared spectroscopy as a predictor for shunt requirement during carotid endarterectomy”. Eur J Vasc Endovasc Surg 53:792
Kondov S, Beyersdorf F, Schollhorn J, Benk C, Rylski B, Czerny M, Harloff A, Siepe M (2019) Outcome of near-infrared spectroscopy-guided selective shunting during carotid endarterectomy in general anesthesia. Ann Vasc Surg 61:170–177
Kong J, Li J, Ye Z, Fan X, Wen J, Zhang J, Liu P (2017) Carotid endarterectomy with routine shunt for patients with contralateral carotid occlusion. Ann Thorac Cardiovasc Surg 23:227–232
Krejza J, Arkuszewski M, Kasner SE, Weigele J, Ustymowicz A, Hurst RW, Cucchiara BL, Messe SR (2006) Carotid artery diameter in men and women and the relation to body and neck size. Stroke 37:1103–1105
Kretz B, Abello N, Astruc K, Terriat B, Favier C, Bouchot O, Brenot R, Steinmetz E (2012) Influence of the contralateral carotid artery on carotid surgery outcome. Ann Vasc Surg 26:766–774
Kretz B, Abello N, Bouchot O, Kazandjian C, Beaumont M, Terriat B, Bernard A, Brenot R, Steinmetz E (2014) Risk index for predicting shunt in carotid endarterectomy. Ann Vasc Surg 28:1204–1212
Li J, Shalabi A, Ji F, Meng L (2017) Monitoring cerebral ischemia during carotid endarterectomy and stenting. J Biomed Res:31
McCarthy RJ, McCabe AE, Walker R, Horrocks M (2001) The value of transcranial doppler in predicting cerebral ischaemia during carotid endarterectomy. Eur J Vasc Endovasc Surg 21:408–412
Moritz S, Kasprzak P, Arlt M, Taeger K, Metz C (2007) Accuracy of cerebral monitoring in detecting cerebral ischemia during carotid endarterectomy: a comparison of transcranial doppler sonography, near-infrared spectroscopy, stump pressure, and somatosensory evoked potentials. Anesthesiology 107:563–569
Naftalovich R, Pantin EJ, Denny JT (2015) Cerebral oximetry decrease after external carotid clamping with normal electroencephalography and no change after internal carotid clamping. A A Case Rep 5:216–218
Orlicky M, Vachata P, Bartos R, Waldauf P, Sames M (2015) A selective carotid artery shunting for carotid endarterectomy: prospective MR DWI monitoring of embolization in a group of 754 patients. J Neurol Surg A Cent Eur Neurosurg 76:89–92
Orlicky M, Hrbac T, Sames M, Vachata P, Hejcl A, Otahal D, Havelka J, Netuka D, Herzig R, Langova K, Skoloudik D (2019) Anesthesia type determines risk of cerebral infarction after carotid endarterectomy. J Vasc Surg 70:138–147
Rerkasem K, Rothwell PM (2009) Routine or selective carotid artery shunting for carotid endarterectomy (and different methods of monitoring in selective shunting). Cochrane Database Syst Rev CD000190
Rigamonti A, Scandroglio M, Minicucci F, Magrin S, Carozzo A, Casati A (2005) A clinical evaluation of near-infrared cerebral oximetry in the awake patient to monitor cerebral perfusion during carotid endarterectomy. J Clin Anesth 17:426–430
Ritter JC, Green D, Slim H, Tiwari A, Brown J, Rashid H (2011) The role of cerebral oximetry in combination with awake testing in patients undergoing carotid endarterectomy under local anaesthesia. Eur J Vasc Endovasc Surg 41:599–605
Samra SK, Dy EA, Welch K, Dorje P, Zelenock GB, Stanley JC (2000) Evaluation of a cerebral oximeter as a monitor of cerebral ischemia during carotid endarterectomy. Anesthesiology 93:964–970
Sehatzadeh S (2015) Is transient ischemic attack a medical emergency? An evidence-based analysis. Ont Health Technol Assess Ser 15:1–45
von Reutern GM, Goertler MW, Bornstein NM, Del Sette M, Evans DH, Hetzel A, Kaps M, Perren F, Razumovky A, von Reutern M, Shiogai T et al (2012) Grading carotid stenosis using ultrasonic methods. Stroke 43:916–921
Ward A, Ferraris V, Saha S (2012) Carotid endarterectomy with contralateral carotid occlusion: is shunting necessary? Int J Angiol 21:135–138
Funding
The Internal Grant Agency of the Krajská zdravotní provided financial support in the form of a grant (IGA-KZ-2017-1-13). The Health Research Council of the Czech Republic provided a grant NV19-04-00270. The sponsors had no role in the design or conduct of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Ethical Committee of the Krajská zdravotní) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Comments
We have here an outstanding clinical investigation by an experienced carotid surgery group. The study goal was to validate bilateral NIRS CO decreases with neurologic deterioration in awake patients, and thereby to establish a critical NIRS value to indicate the need for indwelling shunt.
The method was well conceived and elegant. Patients were monitored for CO with forehead NIRS monitors, and were also operated under loco-regional anesthesia. In this way the accuracy of the NIRS could be validated, but the shunting decision was actually made by direct observation of the patient for neurological changes.
One hundred and five patients (85%) were stable throughout the CEA, while 20 patients (15%) clinically deteriorated during surgery. The mean drop in the cerebral oximetry after selective ICA clamping in clinically stable patients was 6%, while in patients with clinical deterioration the NIRS decreased by 14.5% (p < 0.05). When the cut-off value for selective shunting was set as a 10% decrease of the ipsilateral cerebral oximetry after selective ICA clamping, the sensitivity of the technique was 100% and the specificity 83.0%.
As side observations, female sex and contralateral stenosis/occlusion were significant risk factors for shunt placement.
The series is not completely pure, since for various reasons 5% of the patients were not shunted despite a neurological change suggesting that shunt placement would be beneficial (the unstable group). Four patients (3.2% of the series) in the unstable group suffered strokes; it is unclear whether these patients were the non-shunted patients or shunted patients, but this is of concern.
DWI MRI studies were done postop in 120/125 patents and the results are fascinating. In the group of stable patients (n = 100), they observed a new lesion in 8 (8%). In the patients with clinical deterioration (n = 20), they observed a new ischemic lesion in 11 (55.0%) patients (p < 0.001). Clearly even most patients with DWI lesions were clinically well, but it is interesting and worrisome that patients showed DWI lesions despite successful shunt placement.
My personal technique is somewhat different, and my shunt placement rate is a little higher. I use combined EEG/SSEP monitoring and general anesthesia for CEA. We shunt for any change at all in either EEG or SSEP, or both. With this technique I shunt 15% of patients, and 25% if there is contralateral occlusion, strictly by following the monitoring (1).
The authors conclude that a 10% decrease in the ipsilateral brain tissue oximetry after selective cross-clamping of the ICA provides a reliable cut-off value for selective shunting during CEA. I agree with this, and I believe their study is a true contribution to our knowledge of selective shunting and patient protection for best outcomes.
Christopher Miranda Loftus
PA, USA
1. Loftus CM: Carotid Artery Surgery: Principles and Technique. 2nd edition. New York, Informa Publishing 2006.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Vascular Neurosurgery - Ischemia
Rights and permissions
About this article
Cite this article
Hejčl, A., Jiránková, K., Malucelli, A. et al. Selective internal carotid artery cross-clamping increases the specificity of cerebral oximetry for indication of shunting during carotid endarterectomy. Acta Neurochir 163, 1807–1817 (2021). https://doi.org/10.1007/s00701-020-04621-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-020-04621-1